Ear infections in adults are less common than in children but often more complicated. Symptoms like ear pain, pressure, and muffled hearing can signal otitis media or outer ear infection — and the right treatment depends on which type you have.
Need Care Today?
Get a same-day telehealth visit with a board-certified provider.
Licensed in MD, WA & DE
Book a Visit →Types of Ear Infections in Adults
While ear infections are commonly associated with childhood, adults develop them more frequently than many people realize. Understanding the different types helps guide appropriate treatment. The three main categories of ear infections in adults are:
- Otitis media (middle ear infection): Infection behind the eardrum, often following a cold or upper respiratory infection. Fluid becomes trapped in the middle ear space, creating an environment for bacterial growth.
- Otitis externa (outer ear infection / swimmer's ear): Infection of the ear canal, the passage leading from the outer ear to the eardrum. Often caused by water exposure, trauma from cotton swabs, or skin conditions.
- Serous otitis media (fluid in the ear): Accumulation of non-infected fluid behind the eardrum, often related to allergies or eustachian tube dysfunction. This can cause hearing changes and a sensation of fullness without acute pain.
Each type has different causes, symptoms, and treatment approaches. A provider can help determine which type you are experiencing based on your symptoms and history.
Symptoms
Ear infection symptoms in adults can range from mild discomfort to severe pain. The specific symptoms you experience often depend on the type of infection and its severity. Common symptoms to watch for include:
- Ear pain (otalgia) that may be sharp, dull, or throbbing
- A feeling of fullness or pressure in the ear
- Muffled hearing or temporary hearing loss
- Drainage from the ear (clear, yellow, or bloody fluid)
- Itching inside the ear canal (especially with outer ear infections)
- Ringing in the ear (tinnitus)
- Fever, particularly with middle ear infections
- Dizziness or balance problems
- Pain that worsens when pulling on the earlobe (a hallmark of outer ear infections)
In adults, ear pain can sometimes be referred from other sources such as temporomandibular joint (TMJ) disorders, dental problems, or throat infections. If ear pain persists or is accompanied by fever, drainage, or hearing loss, prompt evaluation is recommended.
Common Causes
Ear infections in adults are triggered by a variety of factors. The most common causes include:
- Upper respiratory infections: Colds and flu cause swelling in the nasal passages and eustachian tubes, trapping fluid in the middle ear where bacteria can multiply.
- Allergies: Seasonal or perennial allergies cause chronic eustachian tube inflammation and congestion, increasing the risk of middle ear infections and fluid accumulation.
- Sinus infections: Sinusitis and ear infections frequently occur together because the sinuses, nasal passages, and eustachian tubes are interconnected.
- Water exposure: Swimming, bathing, or humid environments can trap moisture in the ear canal, creating conditions favorable for bacterial and fungal growth (swimmer's ear).
- Cotton swab use: Inserting cotton swabs into the ear canal can cause micro-abrasions, push wax deeper, and disrupt the ear's natural protective barrier.
- Smoking: Tobacco smoke irritates the eustachian tubes and impairs mucociliary clearance, increasing susceptibility to ear infections.
Adults with chronic conditions such as diabetes, immune deficiency, or skin disorders like eczema are also at elevated risk for ear infections and may experience more severe or recurrent episodes.
Middle Ear vs Outer Ear Infections

Middle ear infections cause deep pain, while outer ear infections cause pain when touching the ear.
Distinguishing between middle ear and outer ear infections is important because they require different treatment approaches. Here are the key differences:
Middle ear infections (otitis media) develop behind the eardrum. They typically follow a cold or respiratory illness and are caused by bacteria or viruses that travel through the eustachian tube. Symptoms include deep ear pain, muffled hearing, a feeling of pressure, and sometimes fever. The pain tends to be constant and may worsen when lying down. Treatment often involves oral antibiotics for bacterial infections, along with decongestants or nasal steroids to improve eustachian tube drainage.
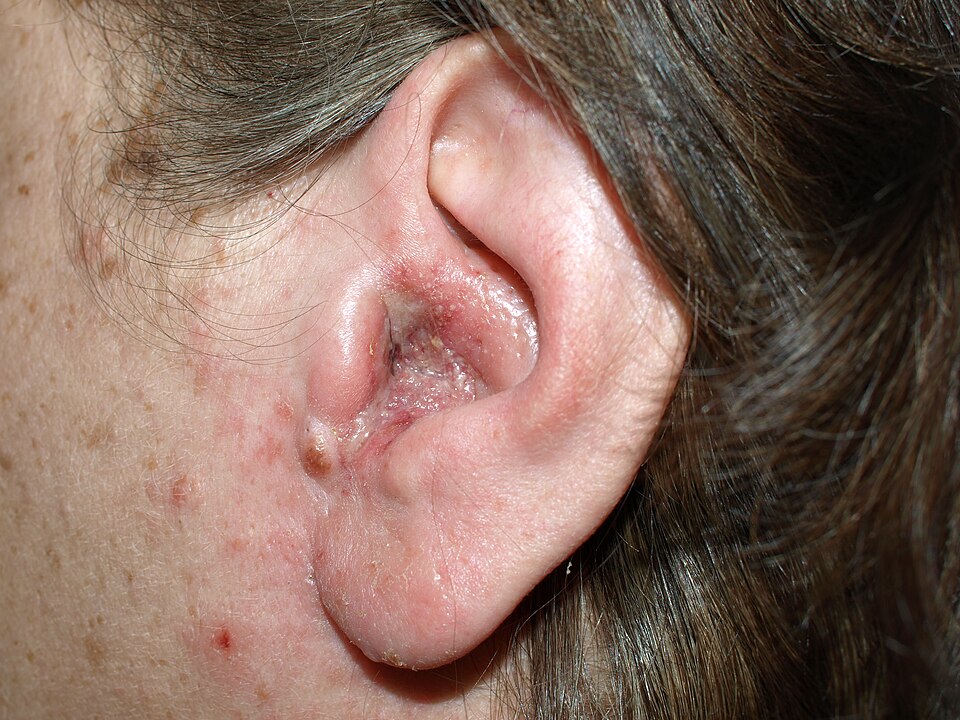
Outer ear infections (otitis externa) affect the ear canal itself. They are often triggered by water exposure, trauma, or skin conditions. The hallmark symptom is pain that intensifies when the earlobe or tragus is pulled or pressed. The ear canal may appear red and swollen, and there may be visible discharge. Itching is common in early stages. Treatment typically involves antibiotic or antifungal ear drops applied directly to the affected canal, and keeping the ear dry during recovery.
A provider can help differentiate between the two based on your symptom pattern, history, and physical description, guiding you toward the most effective ear infection treatment.
Treatment Options
Treatment for adult ear infections depends on the type, severity, and underlying cause. Your provider may recommend one or more of the following approaches:
- Oral antibiotics: Prescribed for bacterial middle ear infections. Common choices include amoxicillin or amoxicillin-clavulanate. A full course is typically 7 to 10 days.
- Antibiotic ear drops: The primary treatment for outer ear infections. Drops containing ciprofloxacin or ofloxacin, often combined with a steroid to reduce inflammation, are applied directly to the ear canal.
- Pain management: Over-the-counter pain relievers such as ibuprofen or acetaminophen can help manage ear pain. Prescription-strength options are available for severe discomfort.
- Decongestants and nasal corticosteroids: These medications help open the eustachian tubes, improving drainage and reducing pressure in the middle ear.
- Antihistamines: When allergies are contributing to eustachian tube dysfunction and recurrent ear problems, allergy treatment can help prevent future episodes.
- Watchful waiting: Some mild ear infections, particularly those suspected to be viral, may resolve on their own within 48 to 72 hours with symptom management alone.
Your provider will tailor the treatment plan based on your specific situation, including any history of recurrent infections or antibiotic allergies.
Home Remedies for Ear Pain
While home remedies cannot cure an ear infection, they can help manage pain and discomfort while you wait for medical treatment or antibiotics to take effect. Safe approaches for temporary ear pain relief include:
- Warm compress: Applying a warm washcloth or heating pad to the affected ear for 15 to 20 minutes can help reduce pain and promote circulation.
- Over-the-counter pain relievers: Ibuprofen and acetaminophen are effective for ear pain. Ibuprofen also reduces inflammation, which can be particularly helpful.
- Elevating the head: Sleeping with your head slightly elevated can help facilitate middle ear drainage and reduce pressure.
- Staying hydrated: Swallowing and yawning help open the eustachian tubes. Drinking fluids and chewing gum can promote this natural drainage mechanism.
Avoid inserting anything into the ear canal, including cotton swabs, ear candles, or home remedy drops unless directed by a provider. Do not attempt to drain the ear yourself. If you have drainage from the ear or a suspected perforated eardrum, avoid getting water in the ear and seek prompt medical attention.
When to See a Provider
Not every episode of ear discomfort requires immediate medical attention, but certain symptoms warrant prompt evaluation. You should see a provider if you experience:
- Ear pain lasting more than 48 hours or worsening despite OTC pain relief
- Fever of 101 degrees F (38.3 degrees C) or higher
- Drainage of fluid or pus from the ear
- Significant hearing loss or sudden hearing changes
- Severe dizziness, vertigo, or balance problems
- Swelling, redness, or pain behind the ear
- Symptoms that develop after swimming or water exposure
- Recurrent ear infections (three or more episodes in a year)
- Ear pain accompanied by severe headache or stiff neck
Seek emergency care immediately if you experience sudden complete hearing loss in one ear, facial weakness or drooping on the affected side, or high fever with severe ear pain and confusion. These may indicate rare but serious complications requiring urgent intervention.
Getting Treatment Online
Telehealth is well-suited for evaluating and treating many adult ear infections. During a virtual visit, your provider will ask detailed questions about your symptoms, their onset and progression, and any associated factors such as recent illness, water exposure, or allergy history. This information, combined with your description of the location and character of your pain, allows accurate assessment in most cases.
Based on the evaluation, your provider can prescribe appropriate medications, including oral antibiotics for middle ear infections or antibiotic ear drops for outer ear infections. Prescriptions are sent directly to your pharmacy for same-day pickup, so you can begin treatment without delay.
InnoCre Telehealth offers same-day ear infection treatment visits for patients in Maryland, Washington, and Delaware. If your provider determines that your condition requires in-person examination, such as cases involving significant drainage, suspected complications, or persistent symptoms despite treatment, they will guide you to the appropriate next step. Getting started is simple: book a visit online and connect with a board-certified provider from the comfort of your home.
Frequently Asked Questions
What causes ear infections in adults?
Adult ear infections are often caused by upper respiratory infections, allergies, sinus infections, or water exposure. Eustachian tube dysfunction from swelling prevents proper drainage.
Can adults get ear infections?
Yes. While more common in children, adults can get both middle ear infections and outer ear infections. Chronic conditions and allergies increase adult risk.
Do I need antibiotics for an ear infection?
Not always. Some ear infections are viral and resolve on their own. Bacterial ear infections may require antibiotics. A provider can help determine the appropriate treatment.
Can a telehealth provider treat an ear infection?
Yes. A provider can evaluate your symptoms, determine the likely type of infection, and prescribe antibiotics or other treatment when appropriate.
How long does an adult ear infection last?
Most adult ear infections improve within 3 to 5 days, with full resolution in 1 to 2 weeks. Outer ear infections treated with antibiotic drops typically clear in 7 to 10 days. Fluid behind the eardrum can linger for several weeks after symptoms resolve.
What's the difference between an outer and middle ear infection?
Outer ear infections (swimmer's ear) affect the ear canal, cause pain when the earlobe is tugged, and are usually treated with antibiotic ear drops. Middle ear infections sit behind the eardrum, follow colds or allergies, cause deep aching pain, and may need oral antibiotics.
Can an ear infection cause vertigo?
Yes. Inflammation in the middle or inner ear can disrupt balance, causing dizziness or true spinning vertigo. Persistent vertigo or sudden hearing loss warrants prompt evaluation to rule out labyrinthitis or other inner-ear conditions.
Why do I keep getting ear infections?
Recurrent ear infections in adults are often driven by untreated allergies, chronic sinus problems, smoking, eustachian tube dysfunction, frequent water exposure, or cotton swab use. Addressing the underlying trigger is key to breaking the cycle.
Can flying with an ear infection cause damage?
Flying with an active middle ear infection can cause severe pain (barotrauma) and, in rare cases, eardrum rupture due to pressure changes. If you must fly, decongestants and chewing gum can help, but it's safer to delay travel until symptoms resolve when possible.
When should I go to the ER for an ear infection?
Go to the ER for sudden complete hearing loss, facial weakness or drooping on the affected side, swelling and redness behind the ear, high fever with severe ear pain, or a stiff neck and confusion. These can signal rare but serious complications.
Sources
Clinical references used in this article:
- Ear Infections. MedlinePlus, National Library of Medicine.
- Hay Fever. MedlinePlus, National Library of Medicine.
- Allergic Rhinitis. MedlinePlus Medical Encyclopedia.
Get the Care You Need Today
A board-certified provider can evaluate your symptoms and recommend treatment. Same-day visits available for patients in Maryland, Washington, and Delaware.
Book a Visit →Visits start at $68 · HSA/FSA accepted · MD, WA & DE
Atul S. Vellappally, DNP, CRNP, FNP-BC
Founder, InnoCre Telehealth. Board-certified Family Nurse Practitioner with doctoral-level training in evidence-based and precision medicine. Licensed in Maryland, Washington, and Delaware.
This article is for informational purposes only and does not constitute medical advice. If you are experiencing a medical emergency, call 911.
Related Services