Many STDs have no symptoms. Learn which STDs are often silent, how to know if you need testing, and how to get tested online.
Need Care Today?
Get a same-day telehealth visit with a board-certified provider.
Licensed in MD, WA & DE
Book a Visit →Why Many STDs Have No Symptoms
The short answer is yes -- you can absolutely have a sexually transmitted disease and not know it. In fact, many of the most common STDs produce no noticeable symptoms at all, especially in the early stages of infection. The organisms that cause these infections -- whether bacteria, viruses, or parasites -- have evolved strategies that allow them to establish themselves in the body quietly, sometimes replicating for weeks or months before triggering any immune response that you would feel.
One reason so many STDs fly under the radar is that they often infect mucosal surfaces like the cervix, urethra, or throat, areas where mild inflammation may not produce pain or visible changes. The body's immune system may mount a low-grade response that keeps the infection somewhat in check without ever producing the classic signs -- discharge, sores, or burning -- that most people associate with an STD. This is why the medical community increasingly uses the term "sexually transmitted infection" (STI) to emphasize that an infection can be present and transmissible long before any disease symptoms appear.
This silent nature of STDs is precisely what makes routine screening so important. Without testing, an asymptomatic infection can be unknowingly passed to sexual partners and, over time, can cause serious health complications. If you are sexually active, regular STD testing is one of the most effective steps you can take to protect both your own health and the health of your partners.
STDs That Are Often Silent
Chlamydia is one of the most frequently asymptomatic STDs. The CDC estimates that roughly 70 percent of women and up to 50 percent of men with chlamydia experience no symptoms whatsoever. When symptoms do appear, they may include mild discharge or a slight burning sensation during urination -- signs that are easy to dismiss or attribute to something else. Left untreated, chlamydia can silently damage the reproductive tract. Chlamydia treatment is straightforward when caught early, typically requiring only a short course of antibiotics.
Gonorrhea follows a similar pattern, particularly in women, where infections of the cervix often produce no symptoms. Men are somewhat more likely to notice urethral discharge or painful urination, but pharyngeal (throat) and rectal gonorrhea are frequently silent in all genders. Human papillomavirus (HPV) is perhaps the most widespread silent STD -- most sexually active adults will contract at least one strain in their lifetime, and the vast majority will never develop warts or other visible signs. Certain high-risk HPV strains can persist for years without symptoms while increasing the risk of cervical, anal, or oropharyngeal cancers. Gonorrhea treatment requires prompt attention, as antibiotic-resistant strains are becoming more common.
Syphilis is sometimes called "the great imitator" because its symptoms, when present, can mimic many other conditions. The initial chancre sore of primary syphilis is painless and often appears in areas that are not easily visible, such as inside the vagina or rectum, so it frequently goes unnoticed. HIV may cause a brief flu-like illness within two to four weeks of exposure, but many people either do not experience this acute phase or mistake it for a common cold. After that initial window, HIV can remain clinically silent for a decade or longer without treatment. Herpes (HSV-1 and HSV-2) can also be asymptomatic or cause such mild outbreaks that they go unrecognized -- studies suggest that up to 80 percent of people with genital herpes are unaware they carry the virus.
How Long Can an STD Go Undetected
The length of time an STD can remain undetected depends on the specific infection. Chlamydia and gonorrhea can be present for weeks to many months without producing symptoms, and if a person is not tested during that time, the infection quietly persists and can be transmitted to partners. trichomoniasis, a parasitic infection, can remain asymptomatic for months or even years -- one study found that some individuals carried the parasite for over a year before diagnosis.
HPV can linger in the body for years or even decades. In many cases, the immune system eventually clears the virus on its own, but high-risk strains can persist and cause cellular changes long before any abnormality appears on a Pap smear or screening test. Syphilis progresses through distinct stages -- primary, secondary, latent, and tertiary -- and the latent stage, during which there are no symptoms at all, can last for years if untreated. A person in latent syphilis may feel perfectly healthy while the bacterium slowly affects internal organs.
HIV has one of the longest asymptomatic windows of any STD. After the potential acute retroviral syndrome in the first few weeks, the virus enters a clinical latency period that can last ten years or more without antiretroviral therapy. During this entire time, the virus is actively replicating and can be transmitted to others. This is why a single negative test does not guarantee long-term safety -- ongoing risk requires ongoing screening.
Risk Factors for Asymptomatic STDs
Anyone who is sexually active can contract an asymptomatic STD, but certain factors increase the likelihood. Having multiple sexual partners or a new sexual partner raises the statistical probability of exposure simply because the pool of potential contacts is larger. Inconsistent condom use is another major risk factor, as barrier methods significantly reduce -- though do not eliminate -- the transmission of most STDs. Younger adults, particularly women under 25, face higher rates of chlamydia and gonorrhea, partly due to biological factors such as cervical ectopy, which makes the cervical tissue more susceptible to infection.
Men who have sex with men (MSM) are at elevated risk for several STDs, including syphilis, gonorrhea, and HIV, and infections at extragenital sites such as the throat and rectum are especially likely to be asymptomatic. A previous STD diagnosis is also a risk factor for future infections, as it may indicate ongoing exposure patterns. Individuals who use alcohol or recreational substances before or during sexual activity may be less likely to use protection consistently, which further increases risk.
It is worth noting that having no symptoms does not mean having no infection. Many people assume they are "clean" because they feel fine, but the absence of symptoms provides no reliable information about STD status. The only way to know for certain is through laboratory testing. If any of the risk factors above apply to you, proactive screening is strongly recommended.
When and How Often to Get Tested
The CDC provides clear screening guidelines that serve as a good baseline. All sexually active women under 25 should be screened annually for chlamydia and gonorrhea. Women 25 and older with risk factors -- such as new or multiple partners -- should also be screened annually. All adults and adolescents aged 13 to 64 should be tested for HIV at least once in their lifetime, and those at higher risk should be tested at least annually. Pregnant individuals should be screened for syphilis, HIV, and hepatitis B at their first prenatal visit, with additional testing for chlamydia and gonorrhea as indicated.
Men who have sex with men should be screened at least annually for syphilis, chlamydia, gonorrhea, and HIV, with more frequent testing (every three to six months) recommended for those with multiple partners. Anyone who shares injection drug equipment should be tested for HIV at least annually. Beyond these guidelines, it is reasonable to get tested whenever you have a new sexual partner, after any unprotected sexual encounter, or if a partner has been diagnosed with an STD.
Keep in mind that each STD has a window period -- the time between exposure and when a test can accurately detect the infection. For example, a chlamydia or gonorrhea nucleic acid amplification test (NAAT) is generally reliable about two weeks after exposure, while fourth-generation HIV antibody/antigen tests may require two to six weeks for accurate results. Your provider can help you determine the right testing timeline based on your specific situation.
How STD Testing Works Through Telehealth
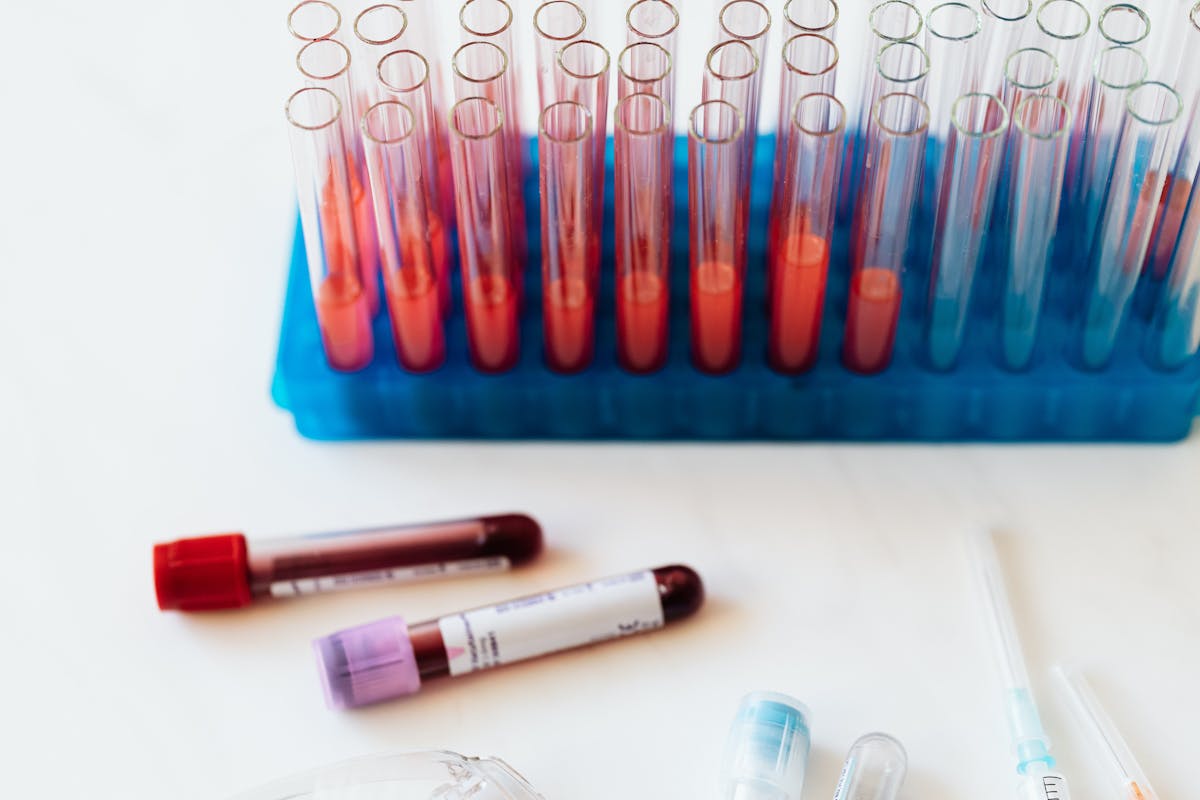
STD testing typically involves a simple blood draw or urine sample at a local lab.
Getting tested for STDs through telehealth is a straightforward process that removes many of the barriers people face with traditional in-office visits. During a telehealth STD consultation, a board-certified provider will review your sexual health history, discuss any risk factors, and determine which tests are appropriate for your situation. This conversation happens through a secure, HIPAA-compliant video visit from the privacy of your own home -- there is no waiting room and no need to take time off work for an office visit.
After your consultation, the provider sends lab orders electronically to a laboratory near you. Most major lab networks, including Quest Diagnostics and Labcorp, have thousands of patient service centers nationwide where you can walk in for a blood draw or urine sample at a time that is convenient for you. STD testing typically involves a simple blood draw for infections like HIV, syphilis, and hepatitis, and a urine sample or swab for chlamydia and gonorrhea. Results are usually available within one to three business days.
If your results come back positive, your telehealth provider can prescribe the appropriate treatment, often during the same visit in which results are reviewed. For bacterial STDs like chlamydia and gonorrhea, treatment is typically a course of antibiotics that can be sent directly to your pharmacy. Your provider can also help you navigate partner notification and answer any questions about follow-up testing to confirm the infection has cleared.
What Happens If an STD Goes Untreated
The consequences of an untreated STD can be serious and, in some cases, irreversible. Untreated chlamydia and gonorrhea are leading causes of pelvic inflammatory disease (PID) in women, a condition in which the infection spreads from the cervix to the uterus and fallopian tubes. PID can cause chronic pelvic pain, scarring of the reproductive organs, ectopic pregnancy, and infertility. In men, untreated chlamydia or gonorrhea can lead to epididymitis, a painful inflammation of the tube behind the testicle that can also affect fertility.
Syphilis follows a particularly concerning progression when left untreated. After the painless chancre of primary syphilis and the rash and systemic symptoms of secondary syphilis, the infection enters a latent phase that can last for years. Eventually, tertiary syphilis can develop, causing damage to the heart, brain, nerves, bones, and other organs. Congenital syphilis -- transmitted from mother to baby during pregnancy -- can cause stillbirth, severe birth defects, and neonatal death, which is why prenatal syphilis screening is so critical.
Untreated HIV progressively weakens the immune system, eventually leading to AIDS if antiretroviral therapy is not initiated. High-risk HPV strains can cause cervical, anal, penile, and oropharyngeal cancers over time. Even herpes, which is often considered a manageable condition, can cause complications in immunocompromised individuals and increases susceptibility to other STDs, including HIV. The good news is that nearly all of these outcomes are preventable with early detection and appropriate treatment. A simple screening test today can spare you years of health complications down the road.
Frequently Asked Questions
Which STDs are most commonly asymptomatic?
Chlamydia, gonorrhea, HPV, and early-stage syphilis are frequently asymptomatic. Up to 70 percent of chlamydia cases in women and 50 percent in men show no symptoms.
How long can you have an STD without knowing?
Some STDs can remain asymptomatic for months or even years. HIV may not cause symptoms for 10 years. Chlamydia and gonorrhea can be silent for weeks to months.
How often should you get tested for STDs?
The CDC recommends annual chlamydia and gonorrhea screening for sexually active women under 25, and for anyone with new or multiple partners. HIV testing is recommended at least once for all adults.
Can a telehealth provider order STD testing?
Yes. A provider can evaluate your risk factors, order appropriate lab work, and prescribe treatment if results are positive. Lab orders can be sent to a local facility near you.
Get the Care You Need Today
A board-certified provider can evaluate your symptoms and recommend treatment. Same-day visits available for patients in Maryland, Washington, and Delaware.
Book a Visit →Visits start at $68 · Insurance accepted · MD, WA & DE
Atul S. Vellappally, DNP, CRNP, FNP-BC
Founder, InnoCre Telehealth. Board-certified Family Nurse Practitioner with doctoral-level training in evidence-based and precision medicine. Licensed in Maryland, Washington, and Delaware.
This article is for informational purposes only and does not constitute medical advice. If you are experiencing a medical emergency, call 911.
Related Services