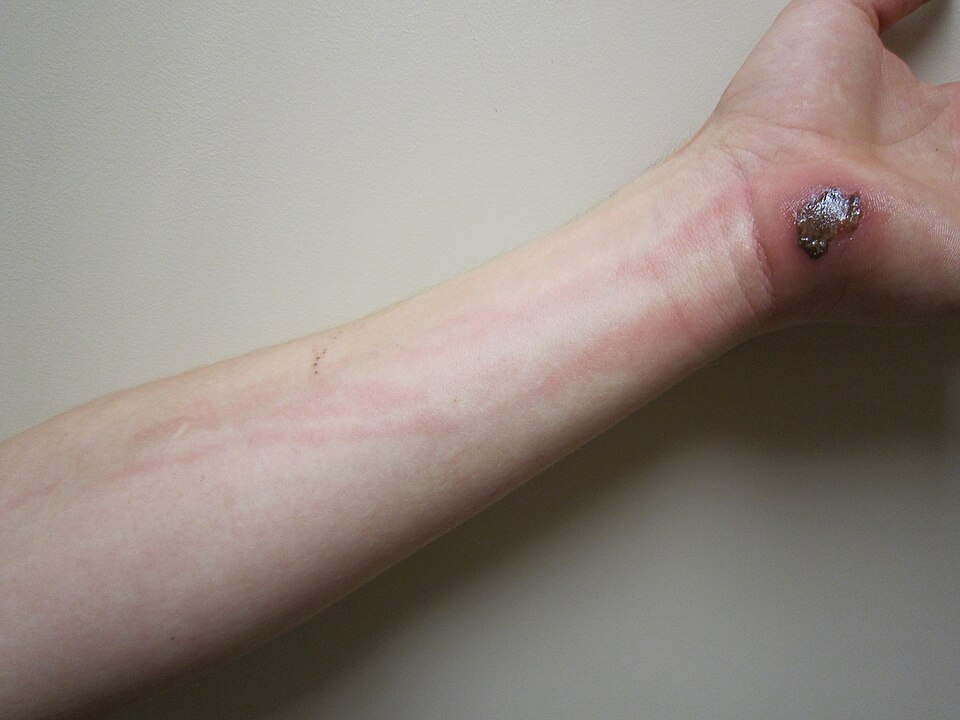
Cellulitis symptoms, how it spreads, treatment with antibiotics, and when to seek emergency care for a skin infection.
Need Care Today?
Get a same-day telehealth visit with a board-certified provider.
Licensed in MD, WA & DE
Book a Visit →What Is Cellulitis
Cellulitis is a common and potentially serious bacterial skin infection that affects the deeper layers of the skin, including the dermis and subcutaneous tissue. It occurs when bacteria enter through a break in the skin, such as a cut, scrape, insect bite, surgical wound, or area of cracked or dry skin. The infection spreads beneath the surface, causing redness, swelling, warmth, and pain in the affected area.
Cellulitis most frequently affects the lower legs, but it can develop anywhere on the body, including the arms, face, and trunk. Unlike superficial skin infections that remain on the surface, cellulitis involves deeper tissue and can spread rapidly if left untreated. Without appropriate antibiotic therapy, the bacteria can enter the bloodstream and cause a life-threatening systemic infection called sepsis.
Cellulitis is not contagious. You cannot catch it from another person through casual contact. However, the bacteria that cause cellulitis are common and can infect anyone who has a break in the skin barrier. Early recognition and prompt treatment are key to preventing complications.
Common Causes
The two most common bacteria responsible for cellulitis are Staphylococcus aureus (including methicillin-resistant strains, or MRSA) and Group A Streptococcus (Streptococcus pyogenes). These bacteria are commonly found on the skin and in the environment, and they take advantage of any disruption in the skin barrier to establish an infection.
Common entry points for bacteria include:
- Cuts, scrapes, and abrasions
- Insect bites or animal bites
- Surgical incisions or IV catheter sites
- Skin conditions that cause cracking, such as eczema, athlete's foot, or severely dry skin
- Ulcers, particularly in patients with diabetes or peripheral vascular disease
- Puncture wounds, including those from stepping on sharp objects
In some cases, no obvious wound or point of entry can be identified. Even microscopic breaks in the skin that are not visible to the naked eye can allow bacteria to penetrate and cause infection.
How to Recognize Cellulitis
Cellulitis typically presents as an expanding area of skin that is red, swollen, warm to the touch, and tender or painful. The redness may spread over hours to days and often has poorly defined, irregular borders that blend into the surrounding normal skin. The affected area may appear shiny and feel tight or firm.
Key signs and symptoms to watch for include:
- Expanding redness that grows larger over time (marking the border with a pen can help you track the spread)
- Skin that is warm or hot compared to the surrounding area
- Swelling and tenderness, especially in the lower leg
- Skin dimpling that resembles an orange peel texture (called peau d'orange)
- Blisters or small pus-filled bumps on the skin surface
- Fever, chills, or body aches, which suggest the infection may be spreading
- Red streaks extending from the infected area toward nearby lymph nodes
Cellulitis can sometimes be confused with other conditions such as contact dermatitis, deep vein thrombosis (DVT), or stasis dermatitis. A provider can help differentiate between these conditions through a clinical evaluation. If you notice spreading redness on your skin, a cellulitis evaluation online can help determine whether antibiotics are needed.
Risk Factors
While anyone can develop cellulitis, certain factors increase your susceptibility to this infection. Understanding your risk factors can help you take preventive measures and seek care early if symptoms develop.
Common risk factors include:
- Previous cellulitis: Approximately 8 to 20 percent of patients who have had cellulitis will experience a recurrence, often in the same location.
- Lymphedema: Chronic swelling caused by impaired lymphatic drainage creates an environment where bacteria thrive and the immune response is diminished.
- Obesity: Excess weight contributes to skin fold moisture, impaired circulation, and lymphatic insufficiency.
- Diabetes: Elevated blood sugar impairs immune function and wound healing, and diabetic neuropathy may prevent patients from noticing small injuries.
- Peripheral vascular disease: Poor circulation slows healing and increases infection risk.
- Skin conditions: Eczema, psoriasis, and athlete's foot create cracks and openings in the skin.
- Immunosuppression: Conditions or medications that weaken the immune system, such as HIV, organ transplant medications, or chemotherapy, increase vulnerability.
- Venous insufficiency: Chronic venous stasis in the legs leads to skin breakdown and swelling.
Treatment with Antibiotics
Cellulitis requires antibiotic treatment. It will not resolve on its own, and delaying therapy increases the risk of complications. The choice of antibiotic depends on the severity of the infection, the suspected bacteria, and your medical history.
For mild to moderate cellulitis without signs of systemic illness, oral antibiotics are the standard first-line treatment. Commonly prescribed antibiotics include cephalexin, dicloxacillin, and amoxicillin-clavulanate for non-purulent cellulitis (without a drainable abscess). If MRSA is suspected, options such as trimethoprim-sulfamethoxazole (Bactrim) or doxycycline may be used instead or in combination.
A typical course of antibiotics for cellulitis lasts 5 to 10 days, though your provider may extend treatment if the infection is slow to improve. Most patients begin to see improvement within 24 to 48 hours of starting antibiotics. It is important to complete the full prescribed course even if symptoms improve before the medication is finished. Stopping antibiotics early can lead to incomplete treatment and recurrence.
In addition to antibiotics, supportive measures include elevating the affected limb to reduce swelling, keeping the area clean and protected, and taking over-the-counter pain relievers such as ibuprofen or acetaminophen for discomfort.
Warning Signs of Severe Infection
While most cases of cellulitis respond well to oral antibiotics, some infections progress to a more severe stage that requires hospitalization and intravenous (IV) antibiotics. Recognizing the warning signs of a worsening infection is critical for getting timely care.
Seek emergency medical attention if you experience any of the following:
- Rapid expansion of redness that spreads noticeably within hours
- Red streaks extending from the infection toward the torso or lymph nodes (lymphangitis)
- High fever (above 102 degrees Fahrenheit), chills, or rigors
- Increased pain that becomes severe or out of proportion to the visible skin changes
- Dark discoloration, blistering, or skin necrosis (tissue death) in the affected area
- Crepitus (a crackling sensation under the skin), which may indicate gas-forming bacteria
- Signs of systemic illness such as rapid heart rate, low blood pressure, confusion, or extreme fatigue
- No improvement or worsening symptoms after 48 hours of oral antibiotic therapy
These signs may indicate that the infection has spread to deeper tissues (necrotizing fasciitis), entered the bloodstream (bacteremia), or is not responding to the current antibiotic regimen. These are medical emergencies that require in-person evaluation and possibly surgical intervention.
Getting Evaluated Online
Telehealth is well suited for evaluating cellulitis, particularly in its early stages. During a virtual visit, your provider can examine the affected area through high-quality video, assess the extent of redness and swelling, and evaluate whether you have systemic symptoms such as fever or chills. Sharing clear, well-lit photos of the affected area before or during the visit can also help with the assessment.
If the evaluation is consistent with mild to moderate cellulitis, your provider can prescribe oral antibiotics, recommend supportive care measures, and schedule a follow-up visit to ensure the infection is improving. Drawing a line around the border of the redness with a pen before your visit allows both you and your provider to track whether the area is expanding or shrinking with treatment.
If your provider determines that the infection appears severe, involves the face, or is not responding to prior treatment, they will direct you to the nearest emergency department or urgent care center for in-person evaluation. At InnoCre Telehealth, same-day appointments are available for patients in Maryland, Washington, and Delaware. Schedule a cellulitis evaluation online or visit our rash treatment page to get started.
Frequently Asked Questions
What does cellulitis look like?
Cellulitis appears as an area of red, swollen, warm, and tender skin that may expand over hours to days. The borders may be blurry. The affected area often feels firm and tight.
Is cellulitis an emergency?
Cellulitis requires prompt antibiotic treatment. Seek emergency care if redness is spreading rapidly, you have a fever, or red streaks are extending from the area toward your heart.
Can cellulitis be treated through telehealth?
Yes. A provider can evaluate photos and video of the affected area, diagnose cellulitis, and prescribe oral antibiotics. If the infection appears severe, they will direct you to in-person care.
How quickly do antibiotics work for cellulitis?
Improvement typically begins within 24 to 48 hours of starting antibiotics. If symptoms worsen or do not improve within 48 hours, contact your provider for reassessment.
Get the Care You Need Today
A board-certified provider can evaluate your symptoms and recommend treatment. Same-day visits available for patients in Maryland, Washington, and Delaware.
Book a Visit →Visits start at $68 · Insurance accepted · MD, WA & DE
Atul S. Vellappally, DNP, CRNP, FNP-BC
Founder, InnoCre Telehealth. Board-certified Family Nurse Practitioner with doctoral-level training in evidence-based and precision medicine. Licensed in Maryland, Washington, and Delaware.
This article is for informational purposes only and does not constitute medical advice. If you are experiencing a medical emergency, call 911.
Related Services